5 years from now, the U.S. Renal Data System predicts, we will nearly double the endstage renal disease population in the United States. With the ongoing struggle to increase organ donation, most of those 650,000 individuals will be on some form of dialysis.
MARTIN OSINSKI, MBA • JAY WISH, MD
Mr. Osinski is president of American Medical Consultants, based in Miami, Fla. He has 21 years experience in recruiting physicians, including 18 years in the nephrology field. Dr. Wish is a professor of medicine and director of the hemodialysis program at University Hospitals of Cleveland.
Physician shortages have been an area of concern and discussion throughout the U.S. health care community for many years, dating back as far as the “Lee and Jones” original needs-based study of the medical workforce in 1933.1 More recently, an article appearing in the Nov. 2, 2004, issue of Annals of Internal Medicine projected a possible shortage of 200,000 physicians in the United States by the year 2025.2 The U.S. Department of Labor likewise projects that the number of health care jobs will increase almost 30% during the next 10 years. Based on these projections, the United States will add more than three million new health care jobs by 2010.
In nephrology, the number of open positions for doctors is already double the number of renal fellows entering practice. What will be the scenario if this nephrologist shortage increases over the next 20 years? How will this shortage affect the way nephrologists practice and what will be the consequences for their patients?
Can anything be done to avert a nephrology workforce crisis?
WHY A SHORTFALL?
The number of nephrologists currently completing training programs in the United States is approximately 340 per year. Recent estimates indicate that approximately 240 nephrologists will be retiring annually over the coming years.3 The net increase of 100 nephrologists per year represents an annual growth rate of slightly over 2%, assuming they would all be going into clinical medicine. With the attraction of careers in pharmaceutical research and other health care business opportunities, that 2% growth is optimistic. The American Medical Association database shows that only 4,900 of the 6,800 nephrologists listed by the AMA are ful-time equivalent clinicians. There are other factors that skew that 2% growth rate even further:
- It is important to recognize that the rate does not reflect the increasing number of female nephrologists entering medical practice. Close to 33% of current nephrology fellows are female. Many are looking for limited working hours and less on-call time, thereby seeing fewer patients than their male counterparts. The authors can attest there are plenty of male renal fellows and nephrologists in practice who would also prefer less on-call time, fewer patients, and fewer working hours. This doesn't bode well for trying to meet future patient growth.
- Although the absolute numbers and percentage have diminished over the past few years, there are still approximately 10% of nephrology fellows in the United States under some visa restrictions that may require them to practice primary care medicine for a few years instead of nephrology.
- There is a growing interest in interventional nephrology among renal fellows in many programs along with continuing interest in transplantation, which restricts some of these physicians from practicing general nephrology.
- There also may be an increase in the number of nephrologists seeking corporate, non-clinical, set-hour positions with pharmaceutical companies, health systems, health plans, and even health care investment advisers. All these factors will contribute to an ever-increasing shortage of nephrologists.
- Recent changes in the Medicare monthly capitated payment rate for nephrologists tie payment to patient visits. While arguments have been made that more “face time” improves patient satisfaction, the new system puts a strain on the thinning ranks of nephrologists.
 …AND THE POPULATION GROWTH
…AND THE POPULATION GROWTH
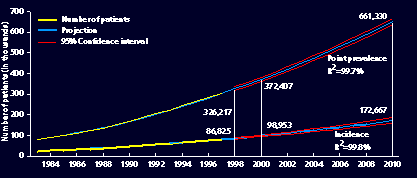
Each year, thousands of new patients begin renal replacement therapy. Current data shows the year-to-year increase in the incident rate is about 5%–7%. But change is expected soon. The U.S. Renal Data System projects the ESRD prevalent population in the United States will exceed 650,000 by the year 2010, up from 350,000 today (see chart). By 2025, the USRDS predicted in its 2003 Annual Data Report, the number of new, or incident cases, could increase by 460,000 per year, with two thirds of these new patients having diabetes as the primary cause of kidney failure. “We project that by 2030, the prevalent population under treatment will reach 2.24 million,” the USRDS stated in its 2004 report.
It is anticipated that the number of patients with chronic kidney disease referred to nephrologists will also increase dramatically due to the aging population; improved awareness by both patients and primary care physicians of the importance of screening at risk populations for CKD; and the effectiveness of nephrologists interventions. The opportunity to identify and aggressively treat CKD in its early stages may help us slow the progress of renal failure; perhaps even prevent it. But payers do not have the right financial incentives in place to treat CKD—and it could drain resources from a shrinking nephrology workforce.
Are nephrologists prepared to deal with these large increases in the patient population? Is there a plan to deal with these shortages on a national level, even from major payers like Medicare, or professional organizations like the Renal Physicians Association, the American Society of Nephrology, and the National Kidney Foundation?
BACKGROUND
Ten years ago, the RPA released a position paper on workforce. Two years later, the Nephrology Workforce Study (cosponsored by the ASN, NKF, RPA, American Society of Pediatric Nephrology, and the American Society of Transplant Physicians), released a followup report. Both papers predicted a severe shortage of nephrologists to meet future patient care demands. Both documents made recommendations to deal with the problem, but little has been done since. The shortages have not changed in any substantial way.
In addition, both studies were done before the “G” payment codes were implemented by the Centers for Medicare & Medicaid Services that tie reimbursement for the monthly capitation rate to the number of face to face nephrologist/patient visits. The RPA Board of Directors commissioned a task force that recently considered the cost/benefit for the organization to formally readdress the workforce issue. The task force concluded that such an effort would be expensive and not likely add new information. An RPA board member noted: “There is an increase in patients, a broadening of procedures, and yet the number of nephrology fellows becoming board certified per year has not changed significantly since the 1997 study.” He predicted things will get worse as the number of ESRD patients per FTE nephrologist increases (projected for 2010 at 140:1 by the RPA study), and necessity grows to utilize extenders. In addition, the RPA task force questioned the value of underwriting a new workforce study when the problems identified in the conclusions of the earlier studies had not yet been addressed.
Mark Rosenberg, MD, chairman of Training Program Directors for ASN, said “meeting manpower needs is the biggest challenge for program directors. It would be necessary for us to train more fellows ourselves,” because most nephrology fellowship programs do not anticipate additional funding to increase capacity. The Balanced Budget Act of 1997 capped the total number of training positions in teaching hospitals. Furthermore, the Accreditation Council for Graduate Medical Education must approve any increase in nephrology training positions, even if a fellowship program can secure additional funding from the hospital, through a shift in residency/fellowship slots or from other sources. “All we can do is make sure we fill all our slots,” Rosenberg said. He mentioned that the ASN will be lobbying for federal legislation to provide additional funding for nephrology training positions, but the association anticipates an unsympathetic Congress. The number of fellows in nephrology has increased since 2001 from 649 fellows (all years) to 780 in 2004. Rosenberg mentioned that the ASN leadership had made similar conclusions to RPA in regards to conducting a new nephrology workforce study: things have changed little since 1997 and the results would be the same. Some programs have added a third year for research to their fellowship, further slowing the flow of fellows to a supply that is in dire need.
It is clear the advent of “G” codes for the dialysis monthly capitation rate; the increased interest in interventional nephrology; the increase in the referral of patients with CKD to nephrologists; the changing specialty demographics which places an increased priority on protected time; and the increase in the number and comorbidities of patients with ESRD will make the need for additional nephrologists only more acute. The role of the nephrologist as the primary care provider for patients with CKD and ESRD will inevitably diminish even more, as the amount of time available to address nonnephrology issues disappears. Continued emphasis has been placed on utilizing physician extenders, such as physician assistants and nurse practitioners, in nephrology practice but there are practical limitations to this strategy. There is a shortage of nephrology extenders, they are expensive, and they are reimbursed at only 85% the rate of a physician for the same services. Nephrology nurse practitioners frequently come from dialysis nursing staffs, exacerbating that shortage.
COMPETITION FROM OTHER SPECIALTIES
Compensation also plays a role in attracting physicians into nephrology. The starting compensation for a nephrologist can be close to half that of an interventional cardiologist. Compensation for nephrologists falls in the middle of the pack when compared to other internal medicine subspecialties. As a rule, cognitive services are undervalued and procedures are overvalued (Pi Center). More has to be done to recognize the value and complexity of nephrology services in order to increase the numbers of the best internal medicine residents going into nephrology. At the same time, public policy (funding and ACGME approved fellowship positions) must allow for an increase in the nephrology trainee pipeline to meet anticipated workforce demands.
The National Institutes of Health’s welcomed emphasis on CKD screening and nephrology referral (through the National Kidney Disease Evaluation Program) needs to be aligned with Medicare funding for the training and reimbursement of nephrologists, who will inevitably be required for CKD outcomes to improve. The projected increase in ESRD patients by 2010 will increase the amount of payments to nephrologists for monthly capitation by over $900 million, totaling more than $2 billion in physician services alone. Since the number of nephrologists is not growing at the same rate, those additional dollars will result in an increase in payments to each nephrologist, unless CMS changes its reimbursement methodology.
Is money enough to attract good doctors into our profession if it means working 24/7? What is the opportunity of going into nephrology if other specialties pay as well for working fewer hours? What about the opportunity of going into medicine at all? The quality of people going into medicine will likely change because generations X, Y, and Z will not work the long hours of previous generations of physicians, even if it means less income. Furthermore, Medicare’s anticipated efforts to hold down health care cost increases in the setting of an aging population with more chronic illnesses, will result in less physician payment for more work. Payment for performance initiatives in medicine may be interpreted as micromanagement and could be another turnoff for the best and brightest in the next generations. Finally, increasing consolidation in the dialysis industry and the prospect of global capitation for ESRD patients may mean that nephrologists will ultimately be employed by health plans or dialysis chains. That is unlikely to be an incentive for productivity in a profession where hard work has traditionally been rewarded with proportionate income.
CONCLUSION
It is not realistic for policy makers to rely on market forces to determine how many individuals enter nephrology practice over the next decade. If the federal government truly takes the coming epidemic of CKD seriously, as it seems to do in Healthy People 2010, then it must allocate the resources to deal with this epidemic prospectively. That includes training the workforce to care for these patients and providing the appropriate economic incentives to maintain that workforce. Reimbursement for evaluation and management services to CKD patients must be adequate to compete with the opportunity costs of a procedure intensive career. ACGME must recognize the impending nephrology workforce crisis by approving more nephrology fellowship positions, and Medicare must allocate funds to support the resulting increase in training costs. We, as a nephrology community, must unite in providing a clear and unambiguous message to Congress and the Department of Health and Human Services that the time to act is now, or the costs of suboptimal CKD care due to an inadequate nephrology workforce will be staggering once these patients reach ESRD. Finally, incentives must be aligned so that patients are not required to overcome barriers to address their CKD and its complications. An inadequate workforce means longer waiting times, further travel, lost educational opportunities, and fragmented care. All stakeholders, including patients, health plans, the government, and health care professionals, will suffer if these issues are not addressed immediately.
REFERENCES
1. Lee RI, Jones LW. The Fundamentals of Good Medical Care. Chicago, Ill.: University of Chicago Press, 1933
2. Cooper, RA. Weighing the evidence for expanding physician supply. Ann Intern Med, 141(11): 705–714, 2004
3. McMurray S. Workforce Issues in Chronic Kidney Disease, presented at American Society of Nephrology annual conference, Philadelphia, Pa., October 2002
This article is reprinted with permission from the March 2005 issue of Nephrology News & Issues.
 (305) 271-9225
(305) 271-9225 Martin Osinski :
Martin Osinski :  NephrologyUSA
NephrologyUSA NephrologyUSA
NephrologyUSA



